Corresponding author: Junki Mizumoto, jnk_mizu@yahoo.co.jp
DOI: 10.31662/jmaj.2021-0079
Received: April 29, 2021
Accepted: September 28, 2021
Advance Publication: December 3, 2021
Published: January 17, 2022
Cite this article as:
Kawasaki MC, Mizumoto J. Hampton’s Hump: Hypoxia with Lung Consolidation Mimicking Pneumonia. JMA J. 2022;5(1):135-136.
Key words: Diagnostic Reasoning, Emergency Medicine, Hampton’s Hump, Pulmonary Embolism, Respiratory Disease
A 72-year-old man presented with mild dyspnea since 1 day prior. He did not experience chest pain, fever, or cough. His vital signs were remarkable in tachycardia, tachypnea, and hypoxia. Chest X-ray revealed slight consolidation at the right lower lung. (Figure 1A) Contrast computed tomography revealed an isolated patchy consolidation at the right lower lobe adjacent with the pleura (Figure 1B and 1C) and multiple defects within the bilateral pulmonary arteries. (Figure 2) The patients was diagnosed with pulmonary embolism (PE). Anticoagulant therapy was administered, and the patient’s conditions improved.
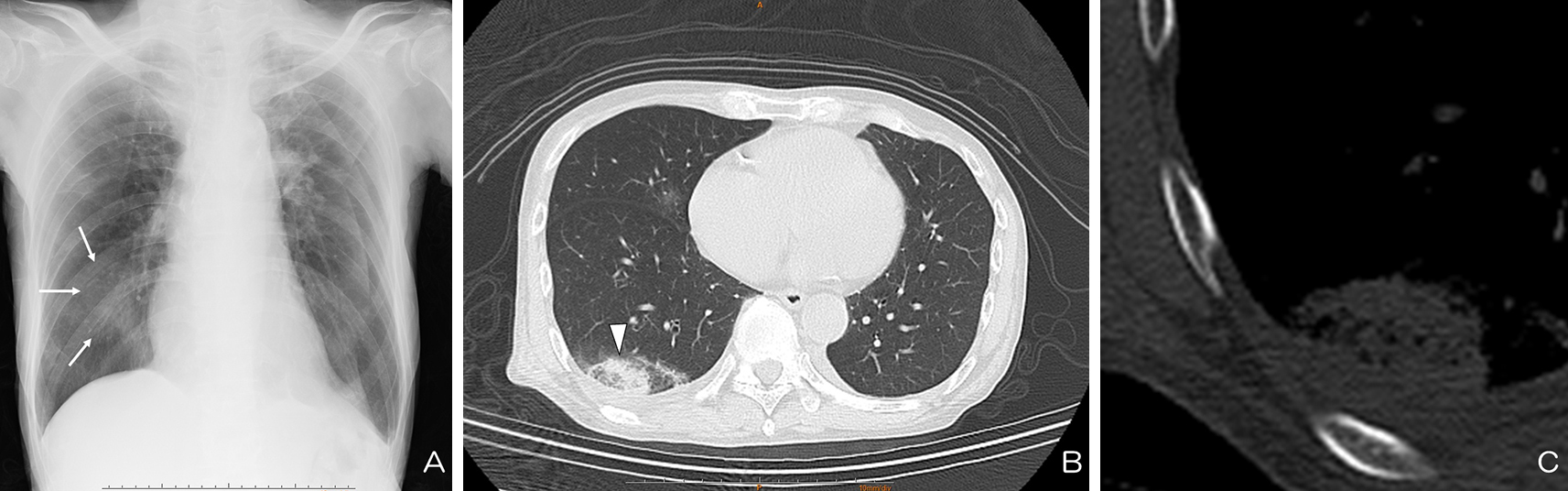
PE sometimes presents with isolated opacity along the pleural surface, called Hampton’s hump (1). It represents small pulmonary infarction. However, it is less frequently seen due to collateral circulation in the lung parenchyma. This sign strongly suggests the presence of PE, although it has low sensitivity (2). Physicians should note that not all consolidations in patients with hypoxemia are due to inflammatory or interstitial disease.
None
Kawasaki CM and Mizumoto J wrote the manuscript.
Informed written consent was obtained from the patient for publication of this report and any accompanying images.
Hampton AO. Correlation of postmortem chest teleroentgenograms with autopsy findings with special reference to pulmonary embolism and infarction. Am J Roentgenol. 1940;43:305-26.
Miniati M, Prediletto R, Formichi B, et al. Accuracy of clinical assessment in the diagnosis of pulmonary embolism. Am J Respir Crit Care Med. 1999;159(3):864-71.