Corresponding author: Kiyozumi Suzuki, kiyozumi.suzuki.med@gmail.com
DOI: 10.31662/jmaj.2021-0180
Received: September 16, 2021
Accepted: October 11, 2021
Advance Publication: December 8, 2021
Published: January 17, 2022
Cite this article as:
Suzuki K, Kanzawa A, Otsuka H, Hirai Y. A Case of Isolated Oral Secondary Syphilis. JMA J. 2022;5(1):139-140.
Key words: secondary syphilis, Treponema pallidum, aphthous ulcers, isolated oral lesions
A 40-year-old man presented to our hospital with a 7-week history of oral lesions with mild pain. He was initially diagnosed with aphthous ulcers by a dentist. Skin and genital lesions were absent, but he disclosed having unprotected intercourse with a female sex worker 5 months before presentation.
Physical examination revealed irregular, whitish ulcerations on the lower lip and tongue (Figure 1 and 2). Rapid plasma reagin [titer: 1:32] and Treponema pallidum hemagglutination were positive, and the HIV test result was negative. Based on a reasonable incubation period, clinical oral findings, and serological tests, a diagnosis of oral secondary syphilis was made. The oral lesions resolved within 1 week of treatment with amoxicillin.
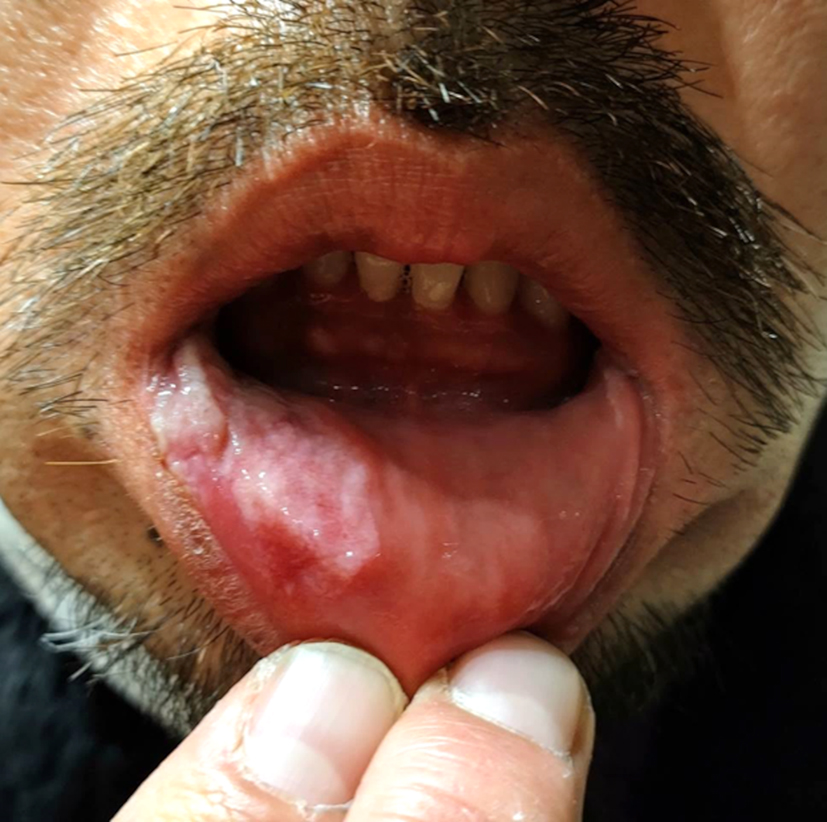
Oral lesions of primary syphilis (so called oral chancres) are typically solitary, painless, indurated ulcers that heal spontaneously within 4-5 weeks (1). In contrast, oral lesions of secondary syphilis are typically painful, multiple, and generally accompanied by cutaneous eruption (1). Isolated oral lesions have been reported to occur in only 7% of patients with secondary syphilis (2), but the condition is potentially underestimated or misdiagnosed (3). Healthcare professionals should consider oral syphilis, including the secondary stage, in the differential diagnosis of isolated oral lesions. A key to early diagnosis and treatment is confirmation of sexual history and prompt syphilis serological testing.
None
Kiyozumi Suzuki: Writing-Original draft, Methodology
Akihiro Kanzawa: Methodology, Writing-review & editing
Hiromasa
Otsuka: Methodology, Writing-review & editing
Yuji Hirai: Methodology, Writing-review & editing
All authors critically reviewed the manuscript.
In this study, IRB approval was not required.
Consent was obtained from the patient for the use of images for publication.
Strieder LR, León JE, Carvalho YR, et al. Oral syphilis: report of three cases and characterization of the inflammatory cells. Ann Diagn Pathol. 2015;19(2):76-80.
Lampros A, Seta V, Gerhardt P, et al. Oral forms of secondary syphilis: an illustration of the pitfalls set by the great imitator. J Am Acad Dermatol. 2021;84(2):348-53.
Zhang W, Mao Q, Lyu X, et al. Diagnosis of oral syphilis remains a challenge-a case report. Int J Infect Dis. 2020;99:231-2.